Sale
Indications
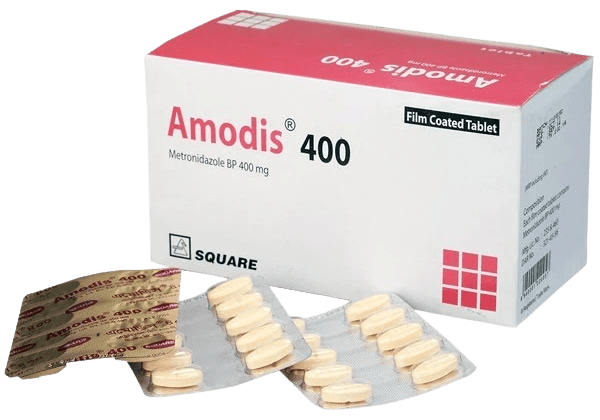
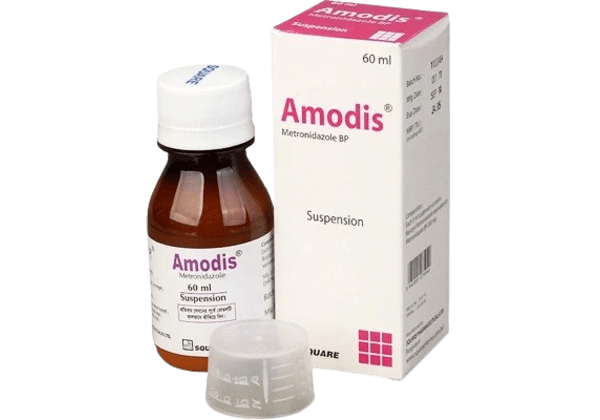
Amodis is indicated in the treatment of following diseases:
The prevention of post-operative infections due to anaerobic bacteria (particularly species of bacteroides and anaerobic streptococci).
The treatment of septicaemia, bacteraemia, peritonitis, brain abscess, pelvic abscess, pelvic cellulitis and post-operative wound infections caused by anaerobes.
Pharmacology
Metronidazole is a member of the imidazole class of antibacterial drug and is classified therapeutically as an antiprotozoal agent. The 5-nitro group of Metronidazole is reduced by anaerobes metabolically. Studies have demonstrated that the reduced form of this drug interacts with DNA and gives bactericidal action of Metronidazole.
Interaction
Disulfiram: Psychotic reactions have been reported in patients who were using Amodis and disulfiram concurrently.
Alcohol: Alcoholic beverages and drugs containing alcohol should not be consumed during therapy and for at least one day afterwards because of the possibility of a disulfiram-like (antabuse effect) reaction (flushing, vomiting, tachycardia). Oral anticoagulant therapy (warfarin type): Potentiation of the anticoagulant effect and increased hemorrhagic risk caused by decreased hepatic catabolism. In case of co-administration, prothrombin time should be more frequently monitored and anticoagulant therapy adjusted during treatment with Amodis.
Lithium: Plasma levels of lithium may be increased by Amodis.
Cyclosporin: Serum cyclosporin and serum creatinine should be closely monitored when co-administration is necessary.
Phenytoin or phenobarbital: increased elimination of Amodis resulting in reduced plasma levels.
5-Fluorouracil: Reduced clearance of 5-fluorouracil resulting in increased toxicity of 5-fluorouracil.
Busulfan: Plasma levels of busulfan may be increased by Amodis, which may lead to severe busulfan toxicity.
Contraindications
Metronidazole is contraindicated in patients with a history of hypersensitivity to Metronidazole or other Nitroimidazole derivatives.
Side Effects
Metallic taste, nausea, vomiting, diarrhoea, drowsiness, rashes may be observed during treatment.
Pregnancy & Lactation
US FDA Pregnancy Category of Metronidazole is B. There are, however, no adequate and well-controlled studies in pregnant women. Because animal reproduction studies are not always predictive of human response, this drug should be used during pregnancy only if clearly needed. Metronidazole have been shown to be excreted in human milk. So, caution should be exercised when Metronidazole is administered to a nursing woman.
Precautions & Warnings
If for compelling reasons, Amodis must be administered longer than the usually recommended duration, it is recommended that hematological tests, especially leucocyte count should be carried out regularly and that patients should be monitored for adverse reactions such as peripheral or central neuropathy (such as paresthesia, ataxia, dizziness, convulsive seizures).
Amodis should be administered with caution to patients with hepatic encephalopathy.
Patients should be warned that Amodis may darken urine.
Use in Special Populations
Hepatic impairment: Amodis is mainly metabolised by hepatic oxidation. Substantial impairment of Amodis clearance may occur in the presence of advanced hepatic insufficiency. Significant cumulation may occur in patients with hepatic encephalopathy and the resulting high plasma concentrations of Amodis may contribute to the symptoms of the encephalopathy. Amodis should therefore, be administered with caution to patients with hepatic encephalopathy. The daily dosage should be reduced to one third and may be administered once daily. Patients should be warned that Amodis may darken urine.
Renal impairment: The elimination half-life of Amodis remains unchanged in the presence of renal failure. The dosage of Amodis therefore needs no reduction. Such patients however retain the metabolites of Amodis. The clinical significance of this is not known at present. In patients undergoing haemodialysis Amodis and metabolites are efficiently removed during an eight hour period of dialysis. Amodis should therefore be re-administered immediately after haemodialysis. No routine adjustment in the dosage of Amodis need be made in patients with renal failure undergoing intermittent peritoneal dialysis (IDP) or continuous ambulatory peritoneal dialysis (CAPD).
Overdose Effects
Single oral doses of Amodis, up to 12 g have been reported in suicide attempts and accidental overdoses. Symptoms were limited to vomiting, ataxia and slight disorientation. There is no specific antidote for Amodis overdosages. In case of suspected massive overdosages, a symptomatic and supportive treatment should be instituted.
Therapeutic Class
Amoebicides, Anti-diarrhoeal Antiprotozoal
Storage Conditions
Store below 30°C. Keep protected from light. Keep medicines out of the reach of children. Do not use later than the date of expiry.